Shift in pediatric medicine allows some heart patients more flexibility and playtime
May 9, 2018, 5:01 PM | Updated: 9:12 pm
SALT LAKE CITY, Utah — There’s a new push in pediatric medicine to make a child’s hospital stay more comfortable and enjoyable for even the sickest patients, and Utah doctors say it helps these kids thrive.
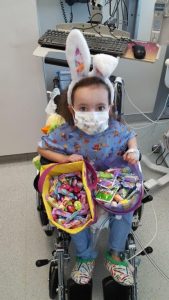
Krista Terry, age 5, spent 194 days at Primary Children’s Hospital waiting for a heart transplant. During that time, she became a trailblazer. She was the first heart patient transferred to a regular floor from the Cardiac Intensive Care Unit.
Michael Profsky, a nurse at Primary Children’s Hospital, said, “It’s real tough. The CICU never sleeps. It’s constantly going. There are lights, there are alarms; there’s no day, no night.”
Moving heart patients who are stable to a main floor is the new standard of care. “It was really good to be up here,” said Paige Terry, Krista’s mom. “She got to be up and out of her bed more. She got to walk around as much as her machine would let her.”
A Berlin heart beat for Krista. It’s a heart pump connected to a machine that maintains blood flow in patients with serious heart failure.
Doctors never know how long a heart transplant patient will be in the hospital waiting for a new heart. It could be a few weeks or up to a year. Now, they can live more of a normal life, and play, which helps them meet developmental milestones.
It was during that time that Krista started her “candy rounds.”
“They made a comment about how it looked like she was on a parade and she needed candy to throw at the nurses,” remembers Terry.
Dr. Lindsay May at Primary Children’s Hospital said, “The patients can leave the room much more freely. They can go to the playroom. We’re able to get them out to the gym, to school, things like that that are more normal and really promote their development.”

Baby Simaya Hem spends time with her family while waiting for a heart transplant at Primary Children’s Hospital.
That’s also been key for another patient, Simaya Hem.
“Good job, high-five,” said her mother, Natalie Hem. A simple moment of play with her 10-month-old daughter on her play mat wouldn’t have been possible before.
She also has a Berlin Heart.
Now, her family can spend time with her all together because along with being healthy enough, there’s plenty of room, which wasn’t possible in the CICU.
“It’s nice because they all come and play and hang out, and they get to go with her for her walks, and stuff like that,” Hem said.
To make the transition work, the nurses did special training, and extra preparations for emergencies.
“We created something called a VAD phone which allowed the nurses to reach a doctor 24-hours-a-day, seven-days-a-week,” said Profsky.

Krista Terry, age 5, does her last “candy rounds” at Primary Children’s Hospital after a successful heart transplant.
May said, “We can have a real-time conversation about the patient. There’s no, ‘I sent a page, no one’s answered.’ There’s not those moments where the nursing staff could feel unsupported or like there’s a potential problem developing.”
After many long months, Krista got a new heart. And it was time for her last candy round. “I’m going home!” Krista Terry said.
For the staff, the moment was bitter-sweet. But definitely more sweet than bitter.