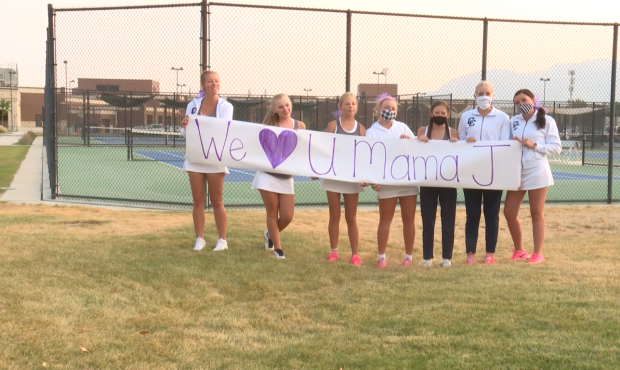COVID-19 Patient Reacts To News That Hospital Resources Could Ration Care
Oct 28, 2020, 9:14 AM | Updated: 9:15 am
SALT LAKE CITY, Utah – The Utah Hospital Association and the Department of Public Safety both say that if the state’s numbers don’t drop soon, hospitals could be forced to activate the Utah Crisis Standards of Care.
Simply put, not all patients will get top priority if resources are maxed out.
Officials said hospitals and staff can’t sustain the current intensive care unit numbers if COVID-19 infections continue to rise. One family who dealt with the reality of the virus firsthand said they can’t imagine getting the news that their loved one couldn’t get care because of a shortage of resources.
Charri Jensen, also knows as beloved Corner Canyon Teacher Mama J, was admitted to the hospital in for COVID-19 in September. She was intubated and spent time in the ICU. She was finally released in early October.
“I wouldn’t wish this on my worst enemy,” she said.
Jensen still needs oxygen to breathe, and her daughter, Talesha, said she couldn’t imagine what would have happened if her mom wouldn’t have had access to critical care.
“To have a doctor or nurse say, ‘Hey, we don’t have enough supplies or equipment to work on your mom,’ — I can’t even imagine,” she said.
The state isn’t to the point that it has to enact its Crisis Standards of Care protocol, but it’s not out of the question if Utah can’t bring its hospitalizations down.
“Right now, we are not in a Crisis of Care,” said Joe Dougherty of the Utah Department of Public Safety. “We are not functioning that way.”
That could change, though.
“Last week we met with the Hospital Association and the chief medical officers of our hospitals,” Dougherty said. “(They) told us in the next week or two, they could be requesting that we invoke Crisis Standards of Care.”
The state’s plan determines which patients get priority for care should it get to the point where there aren’t enough resources to treat everyone.
“It also involves a very specific measurement of who will get the greatest benefit,” Dougherty said. “There’s a whole scoring section.”
Click here to read the full Crisis Standards of Care.
Charri Jensen said she can’t imagine that situation. Despite her challenges, she said she feels fortunate.
“I’m really sad for those that have to go into the emergency room, to the ICU, because it took a village to get me where I am right now,” she said. “I was lucky.”
Talesha Jensen added: “Getting a call from a doctor saying, ‘We don’t have enough equipment,’ I think that would break our family.”
There are a couple of back-up plans in place. First, there are three long-term care facilities that could be used. There is also an option to use the Mountain America Expo Center in Sandy to house non-COVID-19 patients.
However, as health care leaders have been reiterating throughout the pandemic, the number of beds available is a moot number if there aren’t health care workers there to staff them and care for the patients.
Experts said the best option is for the community to bring the numbers down.
The three ways in which to slow the spread of COVID-19 remain constant: Wash your hands often, avoid social gatherings, and wear a mask.