UDOH Includes New Antigen Test Results In Daily Count Of COVID-19 Cases
Jul 17, 2020, 12:23 AM | Updated: 12:30 am
SALT LAKE CITY, Utah – State epidemiologist Dr. Angela Dunn announced 954 new cases of COVID-19 Thursday. If it sounds like too many, that’s because it was — nearly 300 of those cases were from earlier this month, but they were delayed. And 251 of the positive cases were the result of a different method of diagnosis: the antigen test.
“It’s important to let the patient know that there’s a difference between the antigen test and the molecular test,” said Dr. Bert Lopansri, an infectious disease physician at Intermountain Healthcare.
Dr. Lopansri is helping to develop lab tests for COVID-19 at Intermountain. He said the molecular, or PCR test, is what we’re used to. It detects viral RNA and is very accurate. But some labs are getting overloaded with tests and results that should take 48 hours can take up six days.
We spoke to 2 experts on testing who talk about the antigen test, advantages/disadvantages and its impact on Utah’s daily count. @KSL5TV at 10
— Matt Rascon (@MattRasconNews) July 17, 2020
On the other hand, the antigen test “detects the virus with a different perspective and allows us to get the answers sooner,” according to Lopansri.
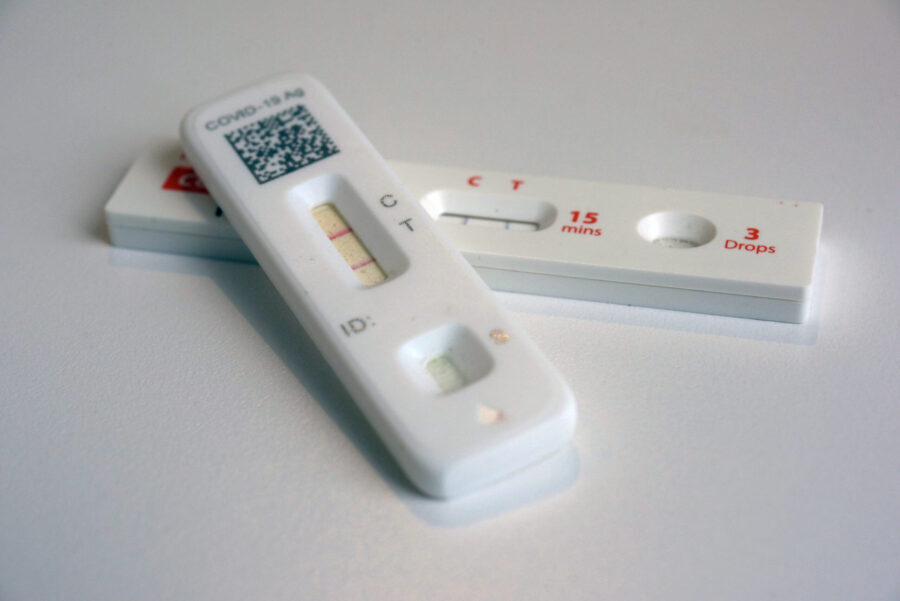
In fact, it only takes the nose swab for the antigen test 15 minutes to detect a protein that’s part of the COVID-19 virus.
“Why antigen tests may have an important role to play is because the current test, molecular tests, are generally very slow. And the turnaround time varies depending on the volume of testing,” Lopansri said.
Still, the antigen has its own drawbacks, which is why the Utah Department of Health didn’t initially include the results. The results date back as far as the beginning of June, during which time health officials have been reviewing the tests’ accuracy.
They’ve now determined it is accurate enough to include in the daily count.
“Because of the nature of the [antigen] test, it doesn’t detect a small amount of viruses as effectively as the molecular tests,” Lopansri said. “It’s not a perfect test. None of the tests available to us are perfect.”
“We made a decision early on that the antigen test is not necessarily the test we want to use for making the diagnosis of the disease,” said Dr. Julio Delgado, chief medical officer at ARUP Laboratories.
Delgado agreed that including positive antigen tests in the state’s total numbers is important, but he said that’s not the case for a negative result from the antigen test, which doesn’t rule out the virus.
“That’s the problem. If you’re negative, depending on the clinical situation, you will have to be tested twice, which obviously adds time to the diagnosis and is not really cost-efficient for that purpose,” Delgado said. “The molecular test is the one that has been used and, in my opinion, it should be the one that continues to be used for the diagnosis.”
Testing has always been a critical component of responding to the virus. It gives health officials the information they need to track the spread and to perform contact tracing to slow the spread. But Lopansri was quick to note, “I think it’s important for everyone to understand that testing is not going to get us out of this.”
Instead, Lopansri said our behaviors – social distancing, wearing masks — are even more important to beat the virus.
“To get past this and to flatten the curve I think we have to be united in our approach and be mindful of each other and do what it takes,” he said.