KSL Investigates Utah’s ability to handle Coronavirus outbreak
Mar 17, 2020, 10:46 PM | Updated: Feb 7, 2023, 3:29 pm
SALT LAKE CITY — As we talk about “flattening the curve” of the novel coronavirus, there is one number that matters most: the number of ventilators and critical care units available to treat critically-ill patients.
The KSL Investigators wanted to know: what’s the capacity of Utah’s hospitals to deal with an influx of serious coronavirus cases?
Preparing Nationally And Locally
Fifteen years ago, the federal government estimated a “moderate pandemic” would require more than 64,000 ventilators. A severe pandemic — like the 1918 flu pandemic — would require 740,000.
In a Johns Hopkins survey completed just last month, it’s estimated our country currently has only 160,000 ventilators: 98,000 basic and 62,000 full-featured.
Depending on the severity of this outbreak, health care workers across Utah may be forced to decide who lives and who dies, when it comes to administering necessary medical equipment to patients in serious need.
Some Utah hospitals, in preparation for the growing pandemic, recently canceled all non-emergent surgeries. Steward Health Care is one of the only major health groups not suspending these surgeries, saying “we are preserving access to scheduled procedure time for as long as possible, and we know that this is crucial for our patients who need surgery to reduce pain or treat a life-threatening condition.”
What Can Utah Health Care Facilities Handle?
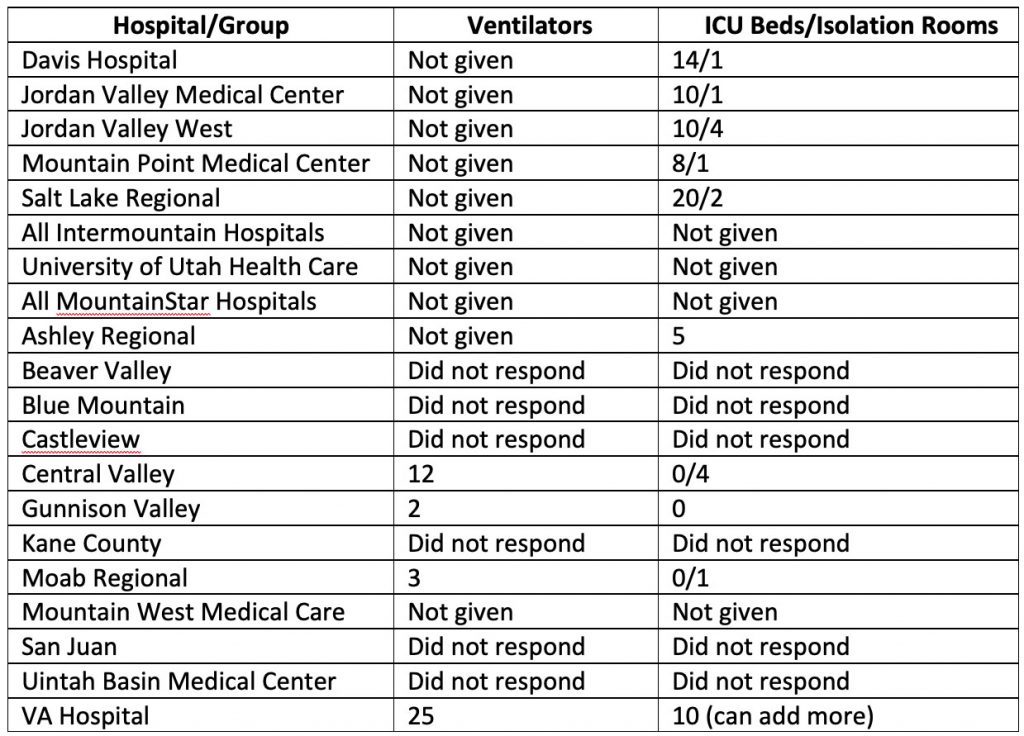
KSL Investigators set out to find out how many ICU beds and ventilators are currently available in the state. We called every hospital and hospital group to find those answers.
Not all were willing to share.
Major health care providers Intermountain Healthcare, University of Utah Health and MountainStar would not release specific data to KSL. Some referred us to the Utah Hospital Association for the tally, who told us to talk to the Utah Department of Health. Our questions to UDOH did not receive an answer.
Rural Utah hospitals were willing to share their data, but their capacity is minimal. Most indicated it would be difficult to keep more than a handful of patients at their facilities. Gunnison Valley Hospital told us with only two ventilators, they would likely be transporting severe cases to larger hospitals along the Wasatch Front.
“We do not have the capacity to handle coronavirus if, in fact, we’re not able to somehow flatten the curve,” said Mike Leavitt, former secretary of Health & Human Services and Utah governor.
Leavitt said spreading out coronavirus cases by flattening the curve would help to prevent overwhelming Utah’s health care system.
“If everyone gets sick at the same time, and we only have a limited number of ventilators, there won’t be enough,” Leavitt said. “I think we’d all like to have the exact numbers, but the reality is this: we don’t have enough ventilators.”
Leavitt said on a federal level, there have been suggestions to have a national backup supply of ventilators but it hasn’t been a priority, which could mean a big difference should the pandemic get worse.
“There will be people who are not treated in the way they should be and it could be the difference between life and death,” Leavitt said.
The national stockpile has an estimated 12,700 ventilators that can be mobilized where needed and the Pentagon announced it will give 2,000 ventilators to the Department of Health and Human Services for coronavirus responses.
Ordering new ventilators will not be a quick fix. Several countries, including China and Italy, have already placed large orders, and manufacturers cannot boost production overnight.
Experts said it could take 90 to 120 days to produce a large order.
Statements From Health Care Groups
Steward Health Care
“As more COVID-19 virus cases are diagnosed in Utah, Steward Health Care is prepared in case we have a surge of patients requiring specific care. Our staff and providers are extensively trained and ready to activate our surge plan to manage a larger number of patients in a safe environment.
System-wide, Steward’s preparations began months ago when the virus initially emerged in the United States. Steward launched a substantial program to acquire and stockpile specialty equipment required to treat COVID-19 patients – including ventilators and personal protective equipment. Many of those resources have been strategically distributed to our hospitals already, as necessary. A significant amount of our resources remains centralized, ready to be deployed or redeployed across our different regions, if and when they are needed.
Because we understand the need to continue to care for sick patients who don’t have COVID-19 – and to keep our emergency rooms as free from COVID-19 as possible, we have instituted remote testing facilities. These remote sites include two “drive-thru” testing centers at Jordan Valley Medical Center and Mountain Point Medical Center, so that suspected patients do not have to go into a hospital setting for testing and risk infecting other patients.
During this pandemic, Steward remains committed — and able — to meet the essential, ongoing health care needs of all our patients.”
MountainStar
“We don’t have specific numbers, but have capacity at each of our eight Utah hospitals to accommodate patients in our ICU with the proper medical equipment.
This is also where being part of HCA Healthcare, one of the largest healthcare systems in the United States, becomes a huge benefit to our patients, caregivers and communities. We have the ability to expand capacity, access to extra beds if needed and most importantly access to the supplies that are so important in these situations. For several weeks, we have been working closely on contingency plans if the need arises to expand capacity. We are ready and will have the resources needed to best care for our community if such a situation.”
University of Utah Health
“Right now, we are directing questions like this to the Utah Hospital Association. We’re not able to share that information at this time.”
Intermountain Healthcare
“Our caregivers are working hard to prepare for the expected surge of cases with planning of appropriate resources and personnel based on experiences in Washington state, New York, and Boston. At this time, we are not releasing specific inventory data.”
VA Hospital
“We have an active and fluid plan in place to add more beds to treat an influx of COVID-19 patients. Our first option will be our acute medicine unit, which is currently empty and is not included in the bed count above.
Additionally, VA Salt Lake City postponed all elective surgeries which frees up critical post-operative and outpatient space for COVID-19 patients. Those employees affected by the changes in surgery schedules will now deploy to areas of the hospital where they are needed most.”
Mountain West Medical Center
“Mountain West Medical Center is a 44-bed hospital with intensive care isolation capabilities. The care and safety of our patients, families, visitors, and staff is our highest priority. Our infection prevention leaders and physicians are carefully monitoring the Coronavirus situation as the outbreak progresses.
We have begun a drive-through screening process and telehealth capabilities that require a call to the hospital, a drive-up to a dedicated entrance or a referral from your primary care provider.
Our community physicians have proactively volunteered their facilities and care in a coordinated manner including Tooele Orthopedics and providers, as well as NorthPointe Ambulatory Surgical Center and their providers.
The hospital has run extensive drills every year preparing for situations like this and the healthcare professionals’ willingness to respond under high pressure is nothing short of heartwarming. We are also coordinating every day with the Tooele Department of Health. We have amazing people in our community.
We follow guidelines from the Centers for Disease Control and Prevention (CDC) for screening, testing, treatment, and infection control.”
Utah Hospital Association
“Unfortunately, as I said, it has been several years since this has been collected by UHA. Like, more than 10.
I did check with UDOH and they don’t collect in the categories requested and it is voluntary reporting, so not good info to put out publicly.
I found a reference to the number of ventilators in Utah in a document prepared a couple of years ago by UDOH and UHA related to emergency response. This document was researched from 2014-2019 and published in 2019. According to this document, there are approximately 600 ventilators available in Utah. There have been new facilities opened since this time so the number is not accurate today.”
Have you experienced something you think just isn’t right? The KSL Investigators want to help. Submit your tip at investigates@ksl.com or 385-707-6153 so we can get working for you.
Coronavirus Resources
- Have you or a family member been affected by coronavirus issues in Utah? KSL TV wants to hear from you. Contact KSL by emailing social@ksl.com.
- What is COVID-19? Here’s What You Need To Know To Stay Healthy
- What We Know And Don’t Know About The Coronavirus
- Four Common Coronavirus Questions Answered
- The latest coronavirus stories from KSL TV can be found at our Staying Safe: Coronavirus section.
- Your Life Your Health: How can parents prepare their home, children against coronavirus?
How Do I Prevent It?
The CDC has some simple recommendations, most of which are the same for preventing other respiratory illnesses or the flu:
- Avoid close contact with people who may be sick
- Avoid touching your face
- Stay home when you are sick
- Cover your cough or sneeze with a tissue and then throw the tissue in the trash
- Wash your hands often with soap and water for at least 20 seconds, especially after going to the bathroom, before eating, and after blowing your nose, coughing or sneezing. Always wash your hands with soap and water if your hands are visibly dirty.
- If soap and water are not readily available, use an alcohol-based hand sanitizer with at least 60% alcohol.
The CDC does not recommend wearing a face mask respirator to protect yourself from coronavirus unless a healthcare professional recommends it.
How To Get Help
If you’re worried you may have COVID-19, you can contact the Utah Coronavirus Information Line at 1-800-456-7707 to speak to trained healthcare professionals. You can also use telehealth services through your healthcare providers.